| Login | ||

Healthcare Training Institute - Quality Education since 1979
CE for Psychologist, Social Worker, Counselor, & MFT!!

Section 4
The Attitudes and Beliefs of Healthcare Professionals regarding
Confidential Reporting and Medication Errors
Question 4
| Test
| Table of Contents
Medication errors are one of the most common types of medical error [1]. It is believed that medication errors may be more common or have more serious outcomes in intensive care units (ICUs) [3]. However, the majority of studies have been in general adult populations; there are very few in the ICU setting.
Medication errors can be broadly divided into prescribing, dispensing and administration errors. There have been two recent studies of prescribing errors in UK ICUs [3, 4]. These reported error rates of 15% [3] and 6.7% [4], with the latter reducing to 4.8% following the introduction of an electronic prescribing system. However, neither sought to explore their causes and there have been no studies of other types of error in UK ICUs.
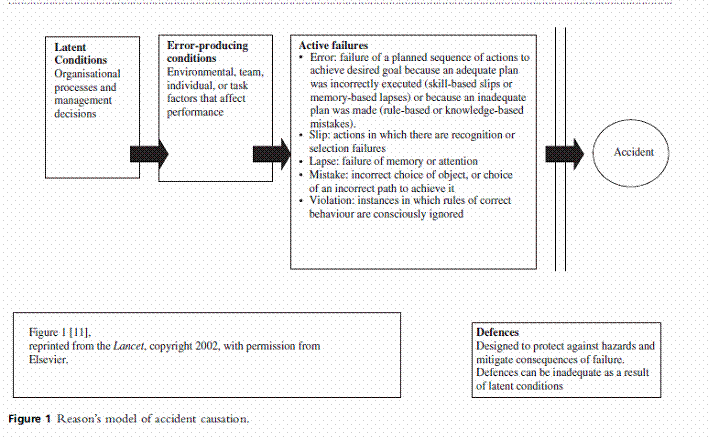
Reason’s Accident Causation Model (Figure 1) [7] is a well-known theoretical framework used to study the causes of errors and accidents in various industries. This approach has also been used to study medical accidents [8–10] and, more recently, prescribing [11] and dispensing [12] errors. However, this approach has not yet been used to study medication errors in an ICU setting. An important issue highlighted in An Organization with a Memory [1] was that mechanisms for reporting and learning from medical errors are generally poor.
Definitions
A prescribing error was defined as a prescribing decision or prescription-writing process that resulted in an unintentional, significant reduction in the probability of treatment being timely and effective or increasing the risk of harm when compared with generally accepted practice [19]. Prescribing without taking into account the patient’s clinical status, failure to communicate essential information, and transcription errors were all considered prescribing errors [19].
Administration errors were defined as any discrepancy between the medication prescribed and that administered to a patient (or omitted) [20]. A documentation error was defined as any situation where a dose of medication was administered correctly but not signed for in accordance with unit policy.
Confidential Interviews
For the non-reported errors, we took a purposive sample with the aim of including errors of a wide range of types and severity grades. Staff were given a participant information leaflet and asked if they would be willing to be interviewed. The information leaflet explained that participants’ identities would be kept confidential and staff willing to take part signed a consent form. To aid recall, we aimed to interview staff within 96 h of the error occurring [11]. Where relevant, we also interviewed nursing staff who administered incorrectly prescribed medication to explore the reasons for the error not being identified at this stage.
Results
About 50 non-reported errors were identified by the pharmacist, all of which were of low or very low severity. Due to the lower than anticipated number of reported errors, a larger purposive sample of 13 non-reported errors was selected to represent a wide range of error types. These comprised six administration errors, six prescribing errors and one documentation error.
Two of the administration errors were identical, relating to the administration of intravenous amiodarone in sodium chloride 0.9% instead of dextrose 5%. The prescriber responsible for the reported prescribing error declined to participate; the remaining 15 members of staff were interviewed. Two interviews could not be analysed due to poor recording quality. We therefore report on the analysis of 13 interviews relating to 12 different errors.
Causes of Errors
The results will be presented according to Reason’s accident causation model, focusing in turn on active failures, error-producing conditions, latent conditions and defenses.
-- Active Failure
There were four slips, one lapse, five mistakes and one violation. The slips were all associated with paying insufficient attention, a classic characteristic of a slip [22]. Lapses were related to memory failure and all mistakes were rule based, relating to lack of knowledge of a relevant rule such as the maximum daily dose of diclofenac, or not knowing that lansoprazole is a proton pump inhibitor.

Error-producing conditions
The most frequent concerned the work environment (six errors). Some staff felt poor communication, either written or verbal, was a factor. One member of staff commented on staff diversity and the variety of accents to contend with. Individual factors, such as physical health and the individual’s knowledge and experience also influenced the occurrence of medication errors. It was evident that one anesthetist was still confused over the maximum dose of a drug.
Defenses
Pharmacists were the main source of defense, and accounted for successful defenses in 10 of 13 errors. Nurses identified and rectified the remaining three. One anesthetist said that not having the pharmacist available at weekends may have contributed to their error not being identified. The nurses were also recognized as a defense, and it was generally accepted by the medical staff that the nurses would check their prescriptions. However, some nurses stated that they would not check the doctor’s prescription, even if they were unfamiliar with doses.
Discussion
This study describes the use of human error theory to identify the causes of prescribing and administration errors in an intensive care unit. We identified many contributing factors. Latent conditions such as the lack of clarity about the responsibility of the second checker, administering medication without a complete prescription and the perceived low importance of double-checking have highlighted issues that were unknown prior to the study.
Previous studies in non-ICU settings [15, 24] suggest that fear of disciplinary action often leads to staff not reporting errors if no harm has come to the patient. Our study also suggests a similar attitude amongst both nurses and anesthetists. Other barriers were also similar to those previously identified [14-17].
--Sanghera, I. S., Franklin, B. D., & Dhillon, S. S. (2007). The attitudes and beliefs of healthcare professionals on the causes and reporting of medication errors in a UK Intensive care unit. Anaesthesia, 62(1), 53-61. doi:10.1111/j.1365-2044.2006.04858.x
Personal
Reflection Exercise Explanation
The
Goal of this Home Study Course is to create a learning experience that enhances
your clinical skills. We encourage you to discuss the Personal Reflection
Journaling Activities, found at the end of each Section, with your colleagues.
Thus, you are provided with an opportunity for a Group Discussion experience.
Case Study examples might include: family background, socio-economic status, education,
occupation, social/emotional issues, legal/financial issues, death/dying/health,
home management, parenting, etc. as you deem appropriate. A Case Study is to be
approximately 100 words in length. However, since the content of these “Personal
Reflection” Journaling Exercises is intended for your future reference, they
may contain confidential information and are to be applied as a “work in
progress.” You will not
be required to provide us with these Journaling Activities.
Personal
Reflection Exercise #4
The preceding section contained information
about the causes and reporting of medication errors. Write one case study example
regarding how you might use the content of this section in your practice.
Reviewed 2023
Update
Reasons for medication administration errors, barriers to reporting them
and the number of reported medication administration errors from
the perspective of nurses: A cross-sectional survey
Brabcová, I., Hajduchová, H., Tóthová, V., Chloubová, I., Červený, M., Prokešová, R., Malý, J., Vlček, J., Doseděl, M., Malá-Ládová, K., Tesař, O., & O'Hara, S. (2023). Reasons for medication administration errors, barriers to reporting them and the number of reported medication administration errors from the perspective of nurses: A cross-sectional survey. Nurse education in practice, 70, 103642. Advance online publication. https://doi.org/10.1016/j.nepr.2023.103642
Peer-Reviewed Journal Article References:
Cipollina, R., & Sanchez, D. T. (2019). Reducing health care disparities through improving trust: An identity safety cues intervention for stigmatized groups. Translational Issues in Psychological Science, 5(4), 315–325.
Keefer, J. M. (2010). Medication literacy. Families, Systems, & Health, 28(4), 392.
Schüz, B., Wurm, S., Ziegelmann, J. P., Warner, L. M., Tesch-Römer, C., & Schwarzer, R. (2011). Changes in functional health, changes in medication beliefs, and medication adherence. Health Psychology, 30(1), 31–39.
Shahidullah, J. D., Hostutler, C. A., & Forman, S. G. (2019). Ethical considerations in medication-related roles for pediatric primary care psychologists. Clinical Practice in Pediatric Psychology, 7(4), 405–416.
QUESTION 4
What is Reason's Accident Causation Model? To select and enter your answer go to Test.
Test
Section 5
Table of Contents
Top
Excerpts from Bibliography referenced in this article
1. Department of Health. Report of an Expert Group On Learning from Adverse Events in the NHS. An Organisation with a Memory. London: The Stationery Office, 2000.
3. Ridley SA, Booth SA, Thompson CM, and the Intensive Care Society’s working Group on Adverse Incidents. Prescription errors in UK critical care units. Anaesthesia 2004; 59: 1193–200.
4. Shulman R, Singer M, Goldstone J, Bellingan G. Medication errors: a prospective cohort study of hand-written and computerised physician order entry in the intensive care unit. Critical Care 2005; 9: R516–21.
7. Reason J. Human Error. Cambridge: Cambridge University Press, 1990.
8. Vincent C, Taylor-Adams S, Chapman EJ, et al. How to investigate and analyse clinical incidents: Clinical Risk Unit and Association of Litigation and Risk Management protocol. British Medical Journal 2000; 320: 777–81.
9. Reason J. Understanding adverse events: the human factor. Clinical Risk Management. London: British Medical Journal Books, 2001: 9–30.
10. Stanhope N, Vincent C, Taylor-Adams SE, O’Connor AM, Beard RW. Applying human factors methods to clinical risk management in obstetrics. British Journal of Obstetrics and Gynaecology 1997; 104: 1225–32.
11. Dean B, Schachter M, Vincent C, Barber N. Causes of prescribing errors in hospital inpatients: a prospective study. Lancet 2002; 359: 1373–8.
12. Beso A, Franklin BD, Barber N. The frequency and potential causes of dispensing errors in a hospital pharmacy. Pharmacy World and Science 2005; 27: 182–90.
14. McArdle D, Burns N, Ireland A. Attitudes and beliefs of doctors towards medication error reporting. International Journal of Health Quality Assurance 2003; 16 ⁄ 7: 326–33.
15. Hand K, Barber N. Nurses’ attitudes and beliefs about medication errors in a UK hospital. International Journal of Pharmacy Practice 2000; 8: 128–34.
16. Jukes AJ, Cavell G. ‘No man is perfect’ – attitudes of healthcare professionals towards the reporting of medication errors in an acute teaching hospital. Pharmacy World and Science 2003; 25: A20–A2.
17. Baker H. Rules outside the rules for administration of medication: a study in New South Wales, Australia. Journal of Nursing Scholarship 1997; 2: 155–8.
19. Dean B, Barber N, Schachter M. What is a prescribing error? Quality and Safety in Health Care 2000; 9: 232–7.
20. Ho CYW, Dean BS, Barber ND. When do medication administration errors happen to hospital inpatients? The International Journal of Pharmacy Practice 1997; 5: 91–6.
22. Reason J. Human error: models and management. British Medical Journal 2000; 320: 768–70.
24. Arndt M. Nurses’ medication errors. Journal of Advanced Nursing 1994; 19: 519–26.

